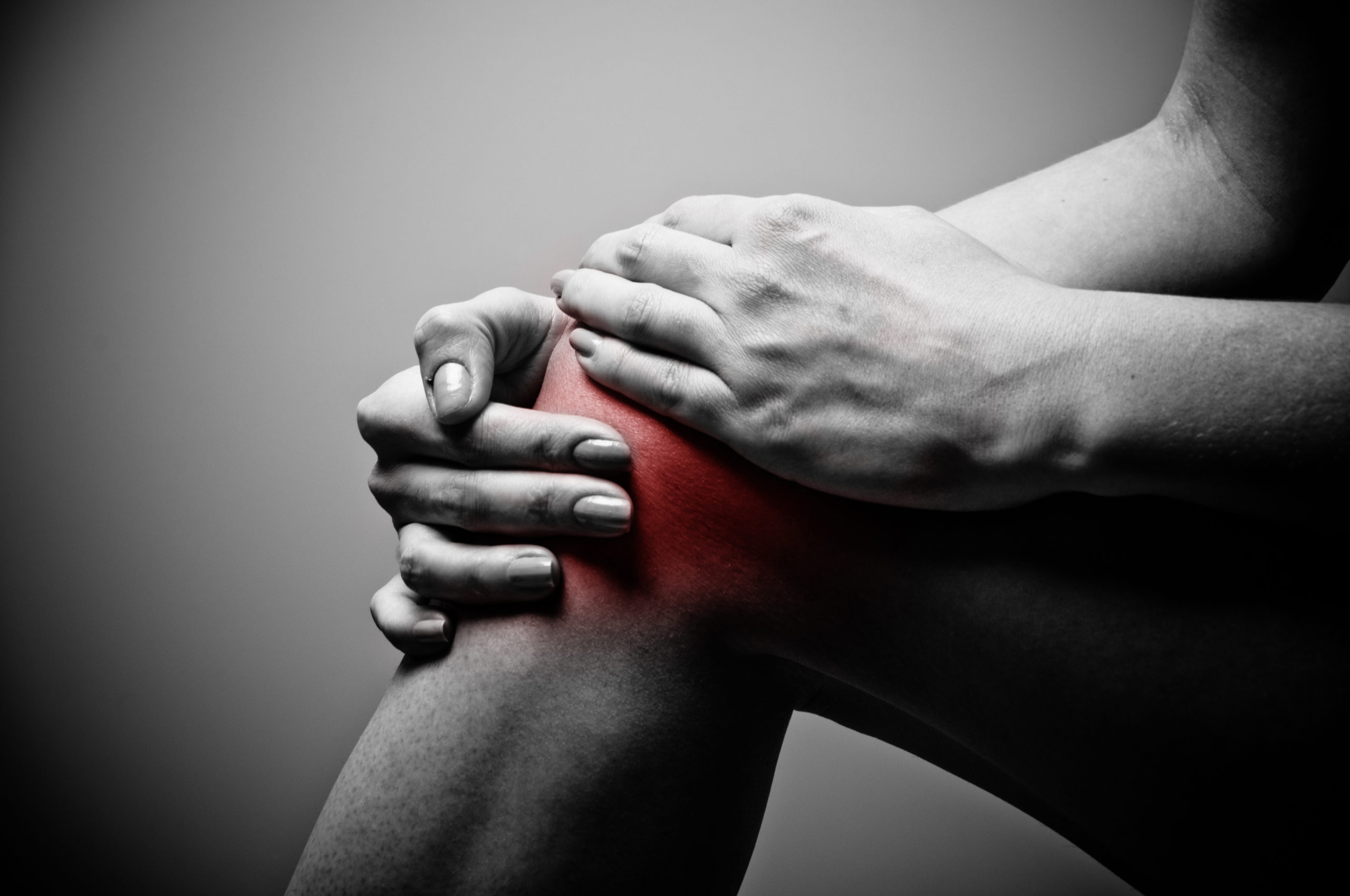
What is osteoarthritis (OA)?
Osteoarthritis is a condition that affects the whole of a joint including bone, cartilage, surrounding soft tissues and muscles. It is a combination of joint degeneration and inflammation. This leads to a reduced ability for the joint to withstand load and move through full range of movement, often leading to the most common symptoms of OA, PAIN and STIFFNESS.
 Osteoarthritis of the knee includes the following physical changes:
Osteoarthritis of the knee includes the following physical changes:
- inflammation of the soft tissues around the knee joint -> often the source of pain
- degeneration/loss of knee joint cartilage -> cartilage is a hard, smooth shock absorbent structure found on the ends of your bones within a joint. This allows a joint to move smoothly and absorb load. There are 3 compartments in the knee the medial and lateral tibiofemoral compartments and the patellofemoral compartment. OA can be isolated to one compartment or in multiple compartments
- reduced size and function of the surrounding muscles most notably the quadriceps muscle group
- changes to underlying bone, including, spurs and cysts
- swelling within the joint
What are the symptoms that indicate you may have knee osteoarthritis?
The primary symptoms of knee OA may vary based to the particular compartment of the knee that is affected however common symptoms include
- pain with weight bearing activities such as climbing stairs, squatting, walking and jogging
- morning pain and stiffness that often eases within an hour. This can also occur after prolonged periods of sitting, such as driving a car or watching television
- inability to completely bend or straighten the knee joint
- weakness or loss of power when trying to push through the affected leg, this can sometimes lead to a feeling of giving way
- a feeling of grinding known as crepitus, locking or instability
What is the cause of knee OA?
Risk factors for developing knee arthritis include both mechanical issues and general health components, these include:
- previous injury to the knee joint, especially those that occur within the joint such as meniscus tears, cruciate ligament injury and joint line fractures
- previous fractures of the adjacent long bones of the thigh and shin
- previous knee surgery
- being overweight or obese -> interestingly this also increases OA in non weight bearing joints such as the wrist, indicating that there are other metabolic factors linking obesity to the development of arthritis in addition to the increased force placed on weight bearing joints.
- sedentary lifestyle including decreased muscle strength and function around the knee joint
- OA in adjacent joints -> hip and ankle
- pre-existing inflammatory conditions such as rheumatoid arthritis or medical conditions that lead to chronic systemic inflammation such as Type 2 Diabetes
How is it diagnosed?
Knee OA is a clinical diagnosis, this means that the diagnosis is made on your history and a thorough physical examination and does not require medical imaging or blood tests. Physiotherapists are highly skilled and trained in making diagnosis of knee arthritis. Diagnosis may also be made by your general practitioner, sports physician, rheumatologist or orthopaedic specialist. Many people will also be referred for a knee x-ray however this is seen as a way of confirming the diagnosis and investigating the degree of degenerative change to the joint cartilage, x-ray findings do not directly determine the management of this condition. Blood tests may also be ordered by your doctor to rule out other forms of arthritis if indicated.
Just a little note on X-RAYS
It is important to remember that degenerative change on x-ray is extremely common and must always be put into context by your treating therapist. An x-ray should be seen as part of the clinical picture and not exclusive of other information such as patient symptoms and function. There are countless examples of people who have degenerative knee changes on x-ray and no symptoms and conversely there are those who have minimal x-ray findings but are suffering symptomatic knee OA. If you have already had a knee x-ray done your physiotherapist will be able to explain and help you understand the radiology report and images.
How can your physiotherapist help you manage knee OA?
The most recent review conducted by the Osteoarthritis Research Society International investigated the most effective non surgical management options for knee arthritis. In broad terms the review investigated treatments such as medication, exercise, electrotherapy, ice/heat, orthotics, bracing, weight loss, education and massage. The authors concluded that the most effective management options for knee OA are
- exercise -> including, weight bearing strength exercises, aerobic conditioning, range of movement exercises and hydrotherapy
- weight loss to reduce load on the knee and decreased inflammation
- education to help patients understand the condition instructions on lifestyle modifications to better manage knee OA
- implementation of walking aids and wedged inner soles if recommended by physiotherapist
- the combined use of medication in conjunction with non-drug therapies listed above led to a better outcome
The major positive is that the most effective treatments are easily accessible, cost effective and achievable for most people. As physiotherapists we have the knowledge to provide the most appropriate tailored exercise program for people managing knee OA, this includes exercise options to assist in weight loss. In conjunction with this we often implement the use of external aids for knee OA such as braces and foot orthoses and are in regular communication with your GP if prescription medication is indicated. Lastly and most importantly we are able to re-assure and educate YOU about knee OA and provide the most relevant information to help you manage your knee pain and dysfunction.
It is important to remember that the ideal management of knee OA often involves various members of your healthcare team including
- general practitioner
- dietician
- podiatrist
- exercise physiologist
- occupational therapist
- psychologist
- orthopaedic specialist
We are lucky to have access to all of these health care experts in the Bargara/Bundaberg region.
If you are concerned you may have knee OA, or have already been diagnosed with this condition and would like to manage it in the most effective way to get the most out of life please contact us on (07) 4159 2904.











